Request An Appointment
Tooth Extractions
Tooth Extractions
- A dental tooth extraction is a procedure where a tooth is removed from its socket in the bone. This is typically done by a dentist or an oral surgeon.
Why Do I Need a Tooth Extraction?
- Tooth Extractions may be necessary for several reasons, including severe decay, fractured tooth, periodontal disease, overcrowding, or to prepare for orthodontic treatment.
What are the Different Types of Extraction?
- Simple Extraction: Typically performed on teeth that are visible in the mouth, using local anesthesia.
- Surgical Extraction: This is more complex and involves teeth that may be broken off at the gum line or have not erupted fully.
Procedure:
- Before the extraction, the dentist or oral surgeon will numb the area around the tooth to be removed.
- Using forceps, the tooth is gently rocked back and forth to loosen it from the jawbone and ligaments holding it in place.
- In some cases, a small incision in the gum and sometimes removal of bone around the tooth may be necessary to facilitate extraction.
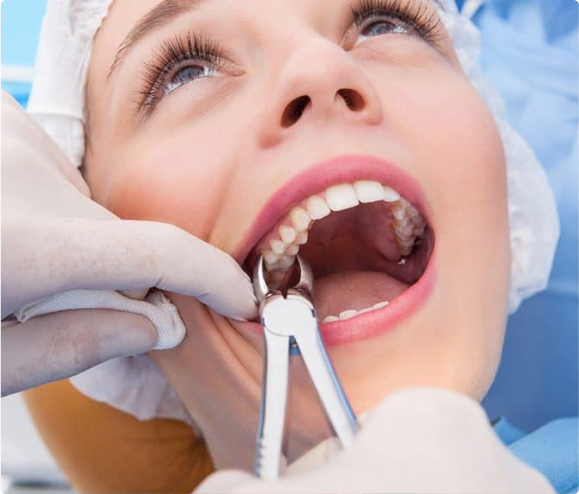

Recommended Additional Treatment After an Extraction:
Bone grafting and guided tissue regeneration.
- Since periodontal disease is the leading cause of bone loss in the oral cavity, bone grafting is a useful procedure for replacing lost bone tissue and stimulating natural bone growth. Bone grafts may be needed to create a stable foundation for the placement of a dental implant, to halt the progression of periodontal disease, and/or even to improve the appearance of your smile. After a tooth extraction and the disease-causing bacteria has been removed from the teeth and roots, bone-grafting material is used to fill the voids in the bone surrounding the teeth. Often bone graft is also combined with tissue-stimulating proteins that help the body regenerate bone and tissue. Tissue regenerative membranes may also be placed over the bone graft to stabilize the graft and further stimulate bone and tissue regeneration.
- Following a tooth extraction, it is generally recommended to place a bone graft into the socket to preserve the bone levels in the mouth, support the ridge, and ultimately make possible a future placement of an implant to replace the tooth that has been removed. Not placing a bone graft after an extraction can limit the options for tooth replacement in the future and result in ridge shrinkage making even a denture more difficult if needed in the future. Your dentist will recommend bone grafting when it is recommended and indicated as it is not always needed.
- After the bone graft is put into the socket the socket is generally closed with sutures. You may need to return in 10-14 days to remove the sutures and check the healing.
Aftercare:
The speed of recovery after you have your wisdom teeth removed depends on how difficult the extraction was. Complete healing usually doesn’t occur for several weeks following the extraction. However, usually within the first week or two, there is enough healing for the area of extraction to feel reasonably comfortable. The dentist will explain exactly what steps you should take following the surgery, but generally here’s what to expect:
- Bleeding may occur for several hours after the extraction. To control it, position a piece of clean moist gauze over the empty tooth socket and bite down firmly. Apply continual pressure for about 45 minutes. A moistened tea bag proves particularly effective because the tannic acid in tea helps healing blood clots to form, functioning similar to scabs over an open wound.
- You should avoid rinsing or spitting for about 24 hours after the procedure and any “sucking” action (like drinking through a straw or smoking). It’s also best to avoid hot liquids like coffee or soup.
- Facial swelling in the area where the tooth was extracted is normal. A piece of ice wrapped in cloth and placed on the swollen area (10 minutes on, 20 minutes off) can help relieve this. After the first 24 hours, treat any facial swelling with heat. Applying a moist warm towel to the swollen area for a 20-minute On, 20-minute Off schedule works well.
- Pain medications, such as acetaminophen (Tylenol) or ibuprofen (Motrin or Advil) can relieve minor pain. The dentist may prescribe more potent pain relievers, as necessary.
- Consume a liquid diet until all the numbness from the anesthesia has worn off followed by soft foods for a few days after that. You should also avoid alcoholic beverages if you’re taking narcotic pain medication.
- Continue to brush your teeth but avoid the teeth close to the extracted tooth during the first 24 hours. Do not use commercial mouth rinses because they can irritate the extraction area.
- Gently rinse your mouth with warm salt water (1/2 teaspoon of salt in a cup of warm water) after meals and before bed starting the second day after the extraction. Again, you should avoid using commercial mouth rinses.
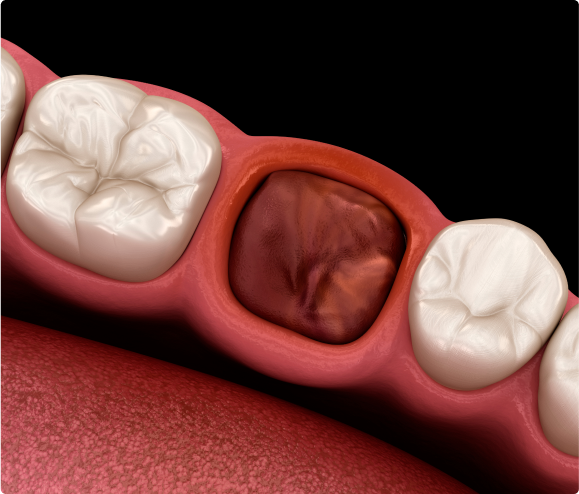
Complications:
While complications are rare, they can include infection, dry socket (when the blood clot breaks down prematurely and is usually a result of excess rinsing and spitting), Sinus exposure, or damage to nearby teeth or nerves.
Recovery:
- Healing typically takes a few days to a few weeks, depending on the complexity of the extraction.
- The gum and bone tissue will gradually fill in the space left by the extracted tooth.
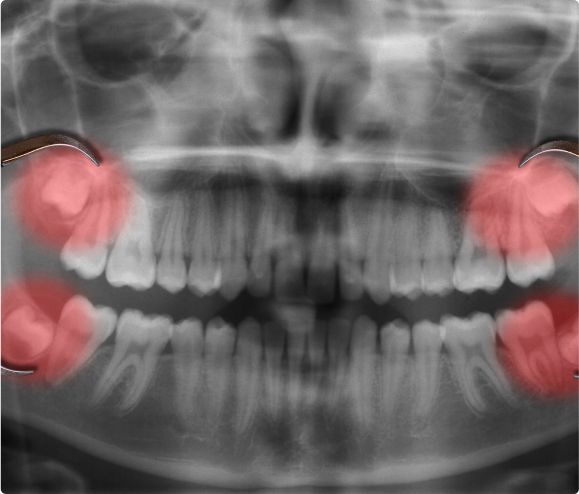
Wisdom Tooth Extractions
- Do you feel a pain in the back of your upper or lower jaw? Have your gums become sensitive in that area? These may be indications that you need your wisdom teeth removed. If so, you shouldn’t procrastinate. Wisdom teeth can cause a great deal of damage to neighboring teeth if you wait too long.
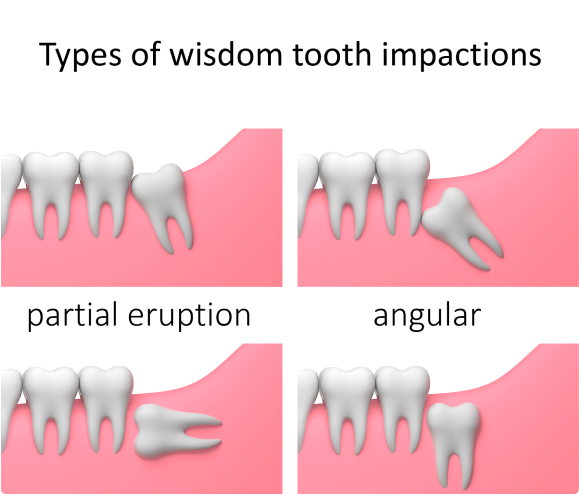
What are Wisdom Teeth?
- A wisdom tooth is any of the four third molars that usually appear in young adults between the ages of 17 and 25. While most individuals have four wisdom teeth, it is possible to have more, in which case they are referred to as “supernumerary teeth.” Some adults do not develop wisdom teeth at all.
- When they are healthy and properly aligned, wisdom teeth can be a valuable asset to the mouth. However, more often than not, they become misaligned (positioned horizontally, angled toward or away from the second molars, or angled inward or outward) and need to be extracted. Even worse, they can crowd or damage adjacent teeth, the jawbone, or nerves.
- Wisdom teeth also can be impacted, which means they become enclosed within the soft tissue and/or the jawbone or only partially break through or erupt through the gum. Partial eruption of the wisdom teeth allows an opening for bacteria to enter around the tooth and cause an infection, which can cause pain, swelling, jaw stiffness, and general illness. Partially erupted teeth are also more prone to tooth decay and gum disease because their difficult-to-reach location and awkward positioning make brushing and flossing difficult.
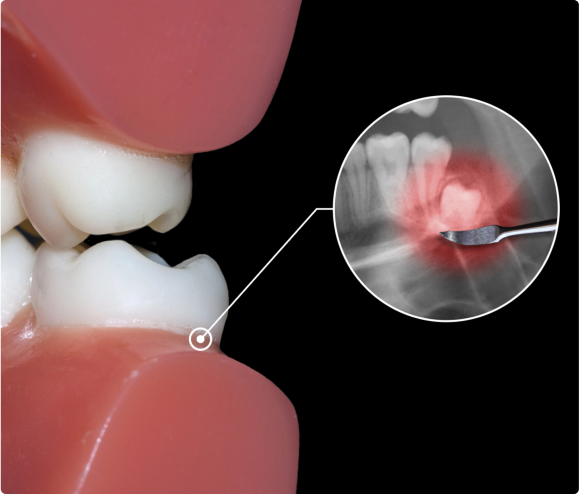
How are Wisdom Teeth Removed?
- The relative ease with which a dentist or oral surgeon can extract wisdom teeth depends on the position of the teeth and their stage of development. A wisdom tooth that has fully erupted through the gum can be extracted as easily as any other tooth. However, a wisdom tooth that is underneath the gums and embedded in the jawbone will require an incision into the gums and then removal of the portion of bone that lies over the tooth. In such cases, the tooth may be extracted in small sections rather than removed in one piece. This minimizes the amount of bone that needs to be removed to get the tooth out.
- Before your wisdom teeth are pulled, the teeth and the surrounding tissue will be numbed with a local anesthetic—the same type used to numb a tooth before you have a cavity filled. In addition to the local anesthetic to numb the pain.
What to Expect Afterwards.
The speed of recovery after you have your wisdom teeth removed depends on how difficult the extraction was. Complete healing usually doesn’t occur for several weeks following the extraction. However, usually within the first week or two, there is enough healing for the area of extraction to feel reasonably comfortable. The dentist will explain exactly what steps you should take following the surgery, but generally here’s what to expect:
- Bleeding may occur for several hours after the extraction. To control it, position a piece of clean moist gauze over the empty tooth socket and bite down firmly. Apply continual pressure for about 45 minutes. A moistened tea bag proves particularly effective because the tannic acid in tea helps healing blood clots to form, functioning similar to scabs over an open wound.
- You should avoid rinsing or spitting for about 24 hours after the procedure and any “sucking” action (like drinking through a straw or smoking). It’s also best to avoid hot liquids like coffee or soup.
- Facial swelling in the area where the tooth was extracted is normal. A piece of ice wrapped in cloth and placed on the swollen area (10 minutes on, 20 minutes off) can help relieve this. After the first 24 hours, treat any facial swelling with heat. Applying a moist warm towel to the swollen area on a 20-minute on, 20-minute off schedule works well.
- Pain medications, such as acetaminophen (Tylenol) or ibuprofen (Motrin or Advil) can relieve minor pain. The dentist may prescribe more potent pain relievers, as necessary.
- Consume a liquid diet until all the numbness from the anesthesia has worn off followed by soft foods for a few days after that. You should also avoid alcoholic beverages if you’re taking narcotic pain medication.
- Continue to brush your teeth but avoid the teeth close to the extracted tooth during the first 24 hours. Do not use commercial mouth rinses because they can irritate the extraction area.
- Gently rinse your mouth with warm salt water (1/2 teaspoon of salt in a cup of warm water) after meals and before bed starting the second day after the extraction. Again, you should avoid using commercial mouth rinses.
The dental surgeons at Crystal Dental Centers have performed many wisdom teeth extractions and can advise you on when’s the right time to get the procedure done. Keep in mind that wisdom teeth can cause a great deal of damage to neighboring teeth if you wait too long. Come in today or schedule an appointment with our office today for a consultation! Contact Us!
10k
Happy Clients
5.0
1,938 Rating
Trusted by 10,000+
happy clients since 2005
Contact Us
Office Hours
| Monday: | 8AM – 5 PM |
| Tuesday: | 8 AM – 5 PM |
| Wednesday: | 8 AM – 5 PM |
| Thursday: | 8AM – 5 PM |
| Friday: | 7AM – 2 PM |
| Sat – Sun: | Closed |
Book An Online Appointment
To schedule an appointment or for more information, complete the form below or call us at 213.748.8448.